Glaucoma Treatment
Glaucoma is an eye disease in which pressure inside the eye (intraocular pressure) rises dangerously high, damaging the optic nerve and causing vision loss. In a healthy eye, fluid is produced in the ciliary body, enters the eye, and then drains through tiny passages called the trabecular meshwork. In people with glaucoma, these passages become blocked and intraocular pressure rises.
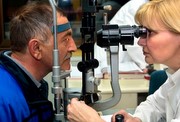
Glaucoma is a leading cause of blindness in the U.S. The condition often develops over many years without causing pain or other noticeable symptoms – so you may not experience vision loss until the disease has progressed.
Sometimes symptoms do occur. These may include:
- Blurred vision
- Loss of peripheral vision
- Halo effects around lights
- Painful or reddened eyes
People at high risk include those who are over the age of 40, diabetic, near-sighted, African-American, or who have a family history of glaucoma.
To detect glaucoma, your physician will test your visual acuity and visual field as well as the pressure in your eye. Regular eye exams help to monitor the changes in your eyesight and to determine whether you may develop glaucoma.
Once diagnosed, glaucoma can be controlled. Some cases of glaucoma can be treated with medications. For others, laser or traditional surgery is required to lower eye pressure.
SLT for Glaucoma
As part of our commitment in offering the best patient care, we are offering the exciting glaucoma therapy Selective Laser Trabeculoplasty (SLT) at Peninsula Eyecare. SLT has revolutionized glaucoma therapy by offering a means to help treat glaucoma without eye drops. SLT uses the low-energy Selecta laser made by Lumenis, Inc., and is performed right here in our office. All you need is a standard appointment; the procedure itself only takes a few minutes.
There are great advantages to using SLT. Here are a few key benefits:
- SLT is not associated with the common side effects of other glaucoma treatments.
- SLT may only need to be administered one time, instead of daily drug regimens.
- SLT takes minutes to perform.
- SLT is not painful.
- SLT replicates the biological response of the body’s own natural process.
- SLT is covered by many insurance companies, including Medicare.
Most important, SLT is a safe and effective treatment. Thousands of eyes have been treated with SLT worldwide. Your eye pressure may drop as soon as a day after SLT. You may be treated with anti-inflammatory eye drops that will be continued after the procedure.
Macular Degeneration Treatment

The macula is a part of the retina in the back of the eye that ensures that our central vision is clear and sharp. Age-related macular degeneration (AMD) occurs when the arteries that nourish the retina harden. Deprived of nutrients, the retinal tissues begin to weaken and die, causing vision loss. Patients may experience anything from a blurry, gray or distorted area to a blind spot in the center of vision.
AMD is the number-one cause of vision loss in the U.S. Macular degeneration doesn’t cause total blindness because it doesn’t affect the peripheral vision. Possible risk factors include genetics, age, diet, smoking and sunlight exposure. Regular eye exams are highly recommended to detect macular degeneration early and prevent permanent vision loss.
Symptoms of macular degeneration include:
- A gradual loss of ability to see objects clearly
- A gradual loss of color vision
- Distorted or blurry vision
- A dark or empty area appearing in the center of vision
Types of AMD
There are two kinds of AMD: wet (neovascular/exudative) and dry (non-neovascular). About 10-15% of people with AMD have the wet form. “Neovascular” means “new vessels.” Accordingly, wet AMD occurs when new blood vessels grow into the retina as the eye attempts to compensate for the blocked arteries. These new vessels are very fragile, and often leak blood and fluid between the layers of the retina. Not only does this leakage distort vision, but when the blood dries, scar tissue forms on the retina as well. This creates a dark spot in the patient’s vision.
Dry AMD is much more common than wet AMD. Patients with this type of macular degeneration do not experience new vessel growth. Instead, symptoms include thinning of the retina, loss of retinal pigment and the formation of small, round particles inside the retina called drusen. Vision loss with dry AMD is slower and often less severe than with wet AMD.
Recent developments in ophthalmology allow doctors to treat many patients with early-stage AMD with the help of lasers and medication.
Macular Degeneration Diagnosis & Treatment
A diagnosis of AMD is made with an examination and a series of tests including an Amsler grid and fluorescein angiography. Fluorescein angiography is the practice of taking photographs of blood vessels inside the eye (an angiogram) with the help of a contrast dye (fluorescein dye). These pictures help doctors evaluate the retina and diagnose problems such as diabetic retinopathy, macular degeneration, abnormal vessel growth, swelling, leaking and retinal detachment.
The latest cutting-edge treatments for wet AMD include:
- MACUGEN – The only FDA-approved treatment for all types of wet AMD. MACUGEN injections are given in a series of treatments spaced six weeks apart.
- Avastin™ – A medication that can reduce swelling in the macula. Avastin is given in a series of injections about 4-6 weeks apart.
- Lucentis – A highly effective drug approved by the FDA in 2006 for the treatment of wet AMD. Lucentis is given in monthly injections.
These revolutionary treatments work by stopping the body from producing VEGF (vascular endothelial growth factor), a chemical that makes abnormal blood vessels grow. The goal of treatment is not only to reduce swelling beneath the macula, but also to preserve and even improve the vision patients have now.
Dry Eye Treatment
Dry eye is a very common disorder of the tear film that results from either decreased tear production or excessive evaporation. The usual signs and symptoms include:
- Burning
- Stinging
- Scratchiness
- Foreign body sensation
- Stringy mucus in or around the eyes
- Excess tearing
- Discomfort when wearing contact lenses
- Fluctuation in vision
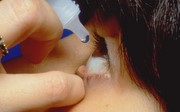
There are many reasons for this condition, such as age (especially women after menopause), use of medications (prescription or over-the-counter) and connective tissues diseases. We can diagnose dry eyes in our office by examining your eyes. Sometimes tests that measure tear production are necessary.
Treatment of dry eyes might include:
- Adding tears by using artificial tears and lubricating ointments.
- Conserving your tears by closing the small opening (punctum) of the channel that connects the eye with the nose. These punctal plugs are made out of plastic and can be used temporarily or permanently. We place the plugs in our office, and the procedure is fast and painless.
- Prescription medication such as:
- RESTASIS to stimulate your own tear production.
- Mild Steroids to reduce inflammation.
- Other methods might include the use of a humidifier, wrap-around glasses, fish oil and more.
Diabetic Retinopathy Treatment
Diabetic Retinopathy is a complication of diabetes that weakens the blood vessels that supply nourishment to the retina (the light-sensitive lining in the back of the eye where vision is focused). These weak vessels can leak, swell or develop thin branches, causing a loss of vision. In its advanced stages, the disease can cause blurred or cloudy vision, floaters and blind spots – and, eventually, blindness. This damage is irreversible.
Fortunately, diabetic retinopathy is preventable. People with diabetes are most susceptible to developing it, but your risk is reduced if you follow your prescribed diet and medications, exercise regularly, control your blood pressure, and avoid alcohol and cigarettes. Regular eye exams are an integral part of making sure your eyes are healthy.
Although damage caused by diabetic retinopathy cannot be corrected, patients diagnosed with the condition can be treated to slow its progression and prevent further vision loss. Treatment modalities include laser and surgical procedures.
Pterygium
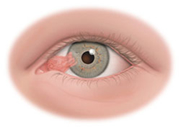
A pterygium is a raised, triangular or wedge-shaped growth of the conjunctiva. It is most common among those who live in tropical climates or spend a lot of time in the sun. Symptoms may include irritation, redness, and tearing.
There is a strong suggestion of a relationship between ultraviolet light exposure (UV) and the development of pterygia during the early years of life and the cumulative exposure over the next 2 to 3 decades in occupations in which there is a high component of reflected ultraviolet light.
Pterygia can affect vision if left unchecked. The corneal degradation may extend beyond the leading edge of the lesion. This means that the pterygium need not cover the visual axis to inflict significant visual compromise. Surgery must be performed before vision is affected.
Peninsula Eyecare Medical Associates has had vast experience in treating pterygium since we are a consultant to the numerous cruise lines visiting Los Angeles. Many of the crew personal are from the tropical areas of the world where pterygium is common and often more complicated.
We have been utilizing a no suture technique that includes an amniotic membrane graft to the area of the pterygium. This makes recurrence much less likely and increases the patient post operative comfort level enormously.
Call our office for an appointment to have your pterygium evaluated and to discuss the possibility of having this new technology incorporated in your safe and successful removal of this unsightly growth.